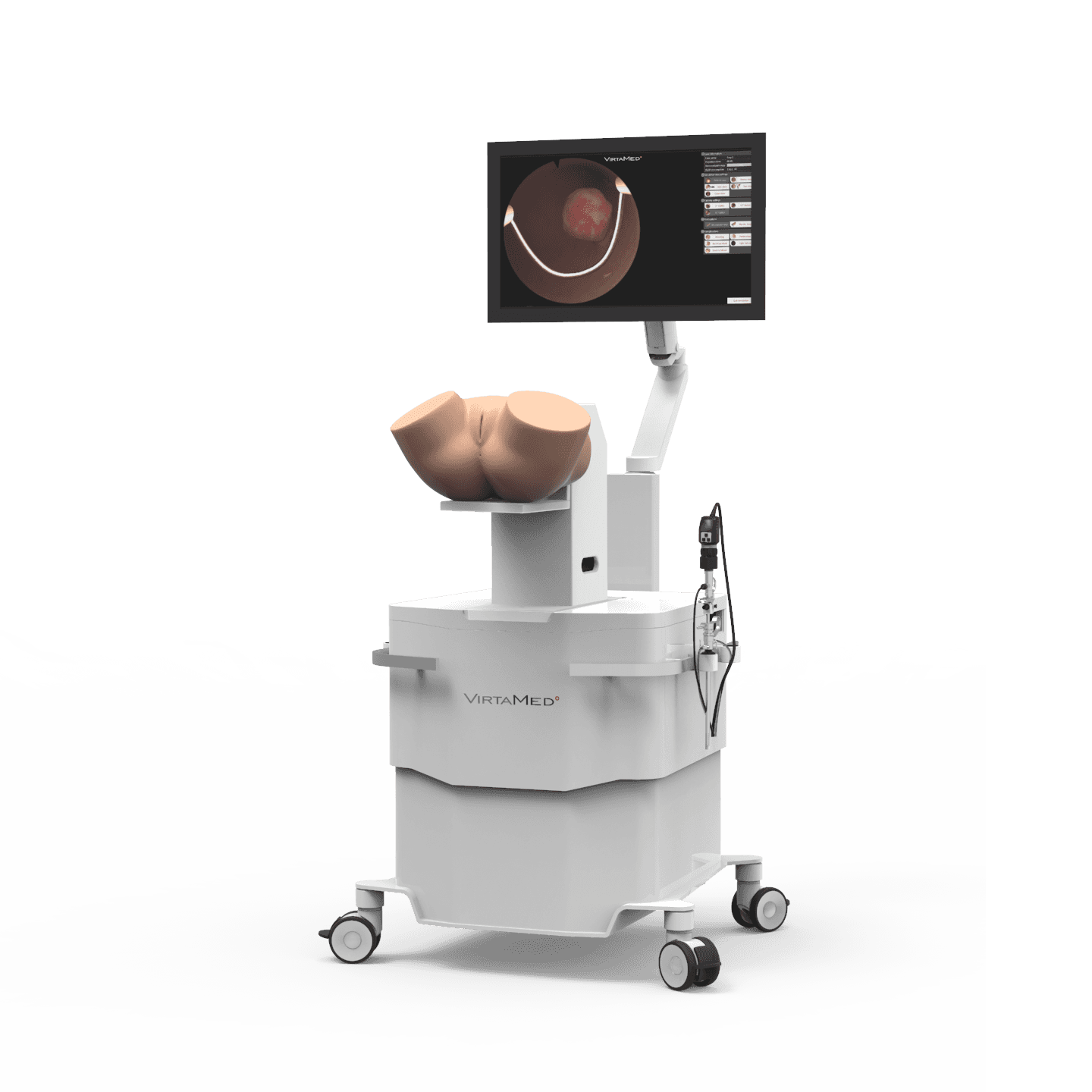
GynoS™
Comprehensive gynecology simulator with unmatched realism: real graphics, real instruments, real feel. Prepare for the operating room with precision and confidence using our state-of-the-art mixed reality technology.
Our expertise
VirtaMed’s immersive training environment, featuring photorealistic graphics and natural haptic feedback, accelerates proficiency while reducing time and costs. VirtaMed’s GynoS™delivers structured,validated training for ob/gyn, ensuring trainees reach defined proficiency levels before real patient interactions. Allows trainees to master pathologies, complications, and critical skills efficiently with dedicated Q&A and reflective opportunities.
Simulation modules
GynoS™ First trimester transvaginal obstetric ultrasound
The realistic tactile feedback from the transvaginal probe helps clinicians transfer their skills from the ultrasound simulator to real patients. Clinicians learn to assess the viability of first-trimester fetuses, including pregnancies of unknown location and ectopic pregnancies, by focusing on fetal ages between 5 and 12 weeks.
GynoS™ Second trimester transabdominal obstetric ultrasound
As the first simulator to incorporate the ISUOG 20+2 scanning protocol, the VirtaMed ultrasound simulator offers the most systematic approach to examining the second-trimester fetus. Equipped with a proprietary probe that allows for free navigation across the entire abdomen, the simulator provides an experience as close to real-life settings as possible.
Clinicians can practice across over 100 cases, including various fetal positions, different placenta locations, and Doppler imaging. Fetal ages range from 20 to 26 weeks.
GynoS™ ASRM embryo transfer simulator and intrauterine insemination
Developed in collaboration with the American Society for Reproductive Medicine (ASRM), the Embryo Transfer simulator is used to train clinicians in embryo transfer for both in vitro fertilization (IVF) and intrauterine insemination (IUI), with and without ultrasound guidance. The simulator combines an anatomically correct pelvic model, original Wallace® and Cook Guardia™ catheters, and a proprietary transabdominal probe. Training cases are based on real patient ultrasound images and include interchangeable uteri and cervix models with unique features, such as straight, bent, and tortuous cervical canals, canals with false passages, and retroverted uteri. The simulator accommodates all three embryo transfer techniques defined by the ASRM: afterload, transfer with trial, and transfer without trial.
GynoS™ Ovum Pick-Up (OPU)
The Ovum Pick Up (OPU) simulator is designed to provide comprehensive training for healthcare professionals, focusing on mastering key aspects of the OPU procedure. The training goals include learning to accurately identify and locate essential anatomical structures, practicing safe puncture techniques, and efficiently aspirating follicular fluid and oocytes. Additionally, the simulator helps develop the motor and coordination skills required to perform the procedure effectively within a team setting.

GynoS™ IUD Placement
A diversity of training cases teach doctors how to safely insert intrauterine devices (IUDs) in either anteverted or retroverted uteri, and in both nulliparous and parous patients. Repeatable cases help trainees quickly master the relevant motor skills while safely handling and correctly placing the IUDs. A patient comfort scale provides immediate feedback on the safety and quality of the procedure. Outside views and ghost tools guide the trainee during their first placements. Trainees can then record and review unguided procedures for debriefing.
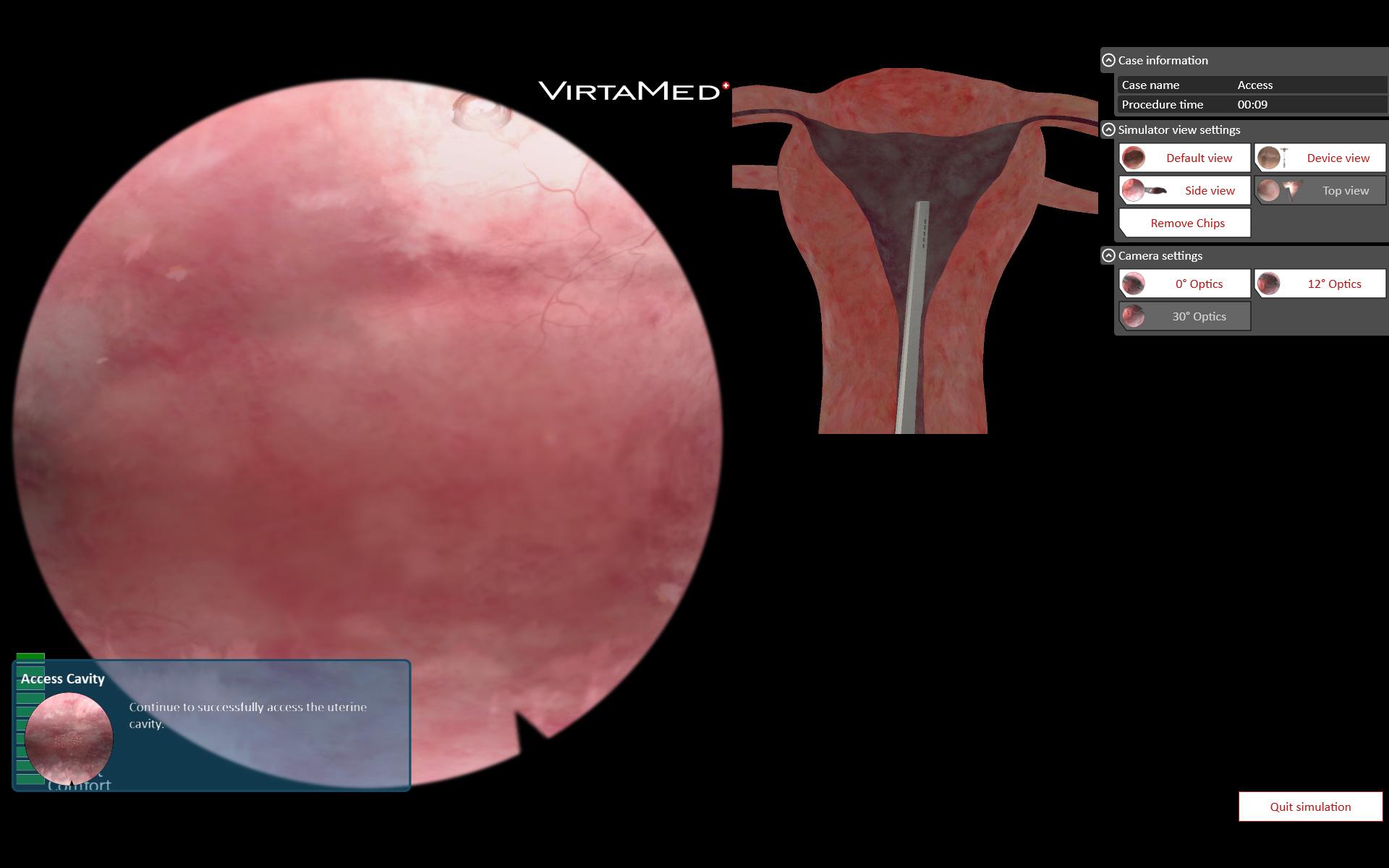
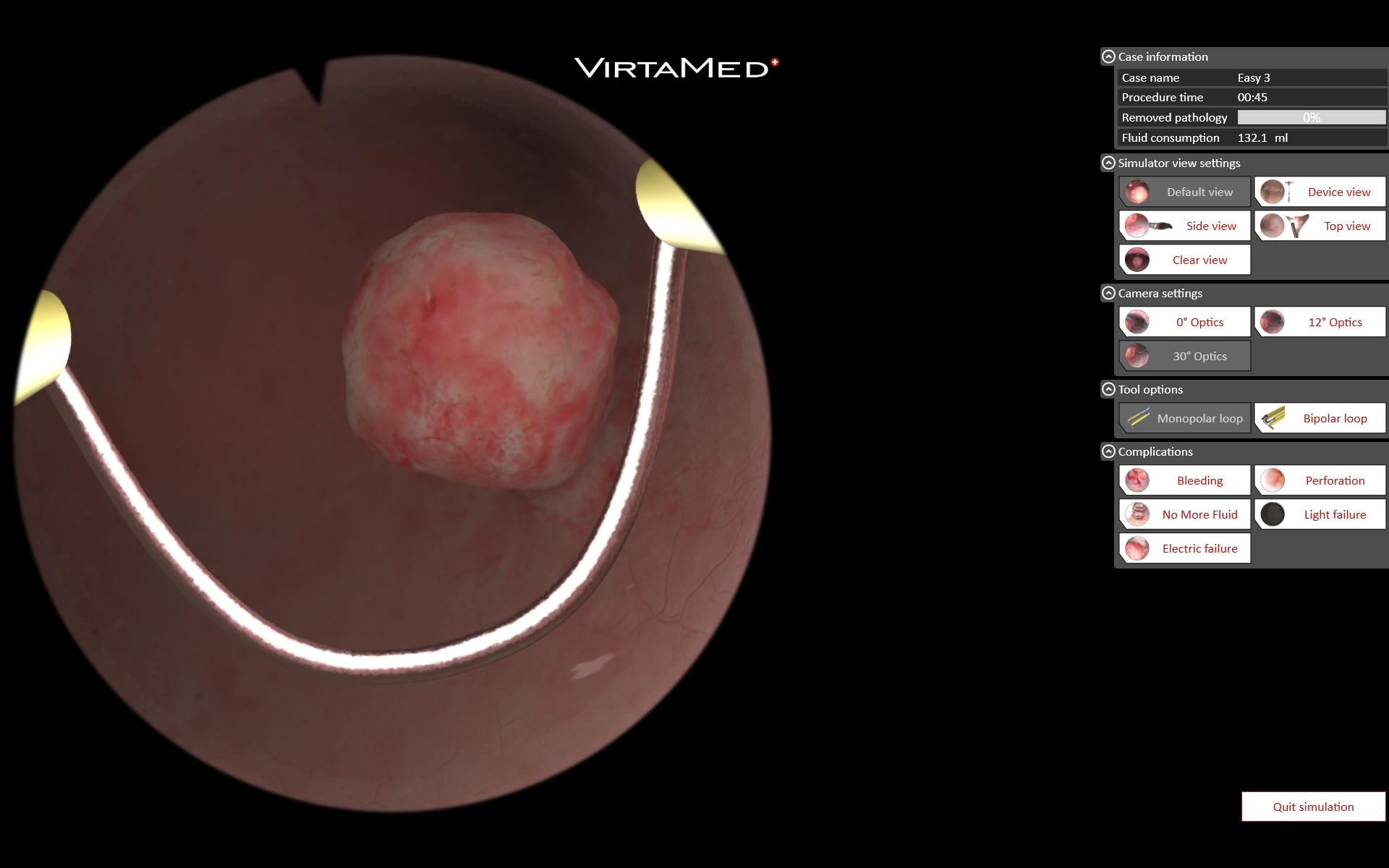
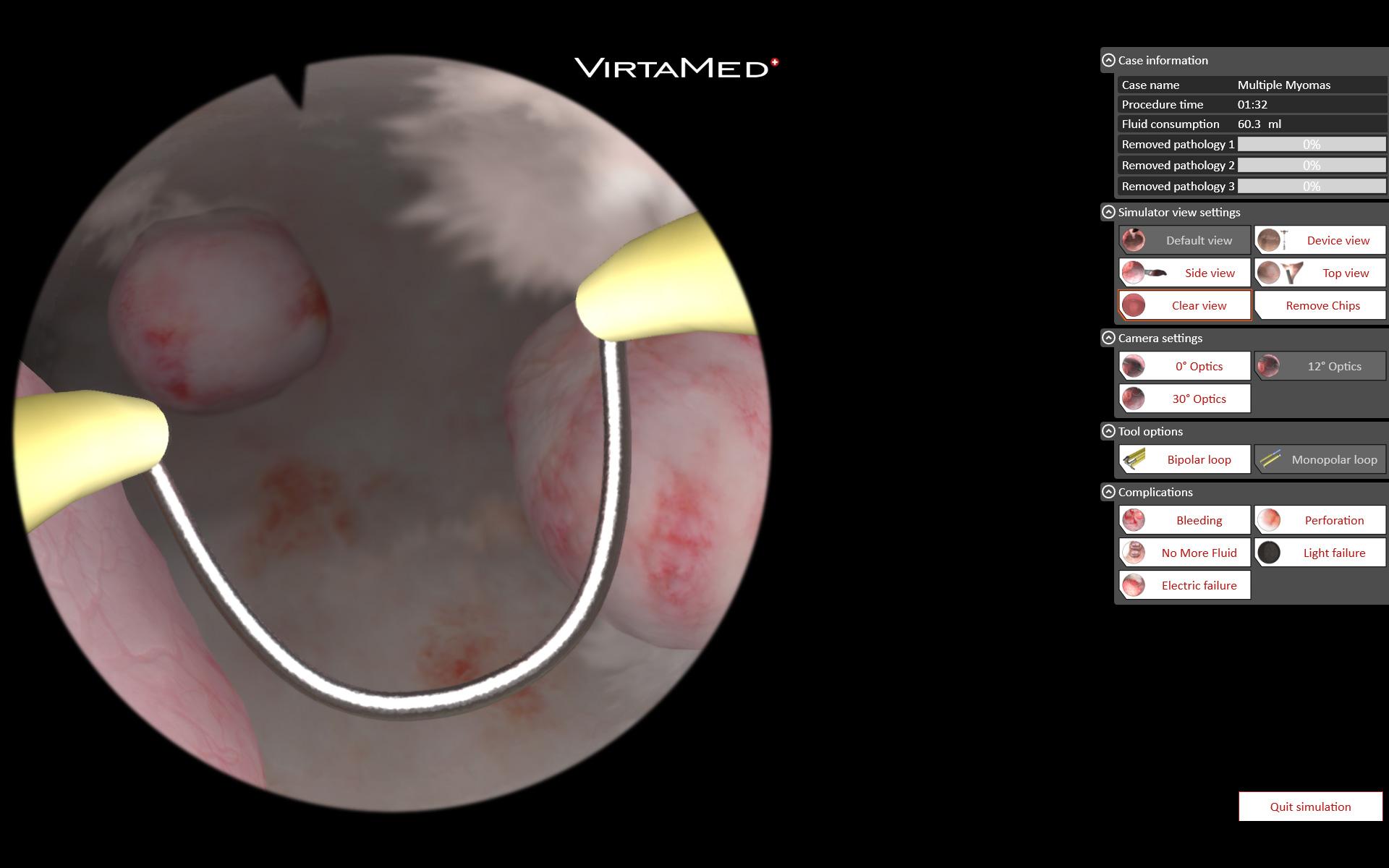
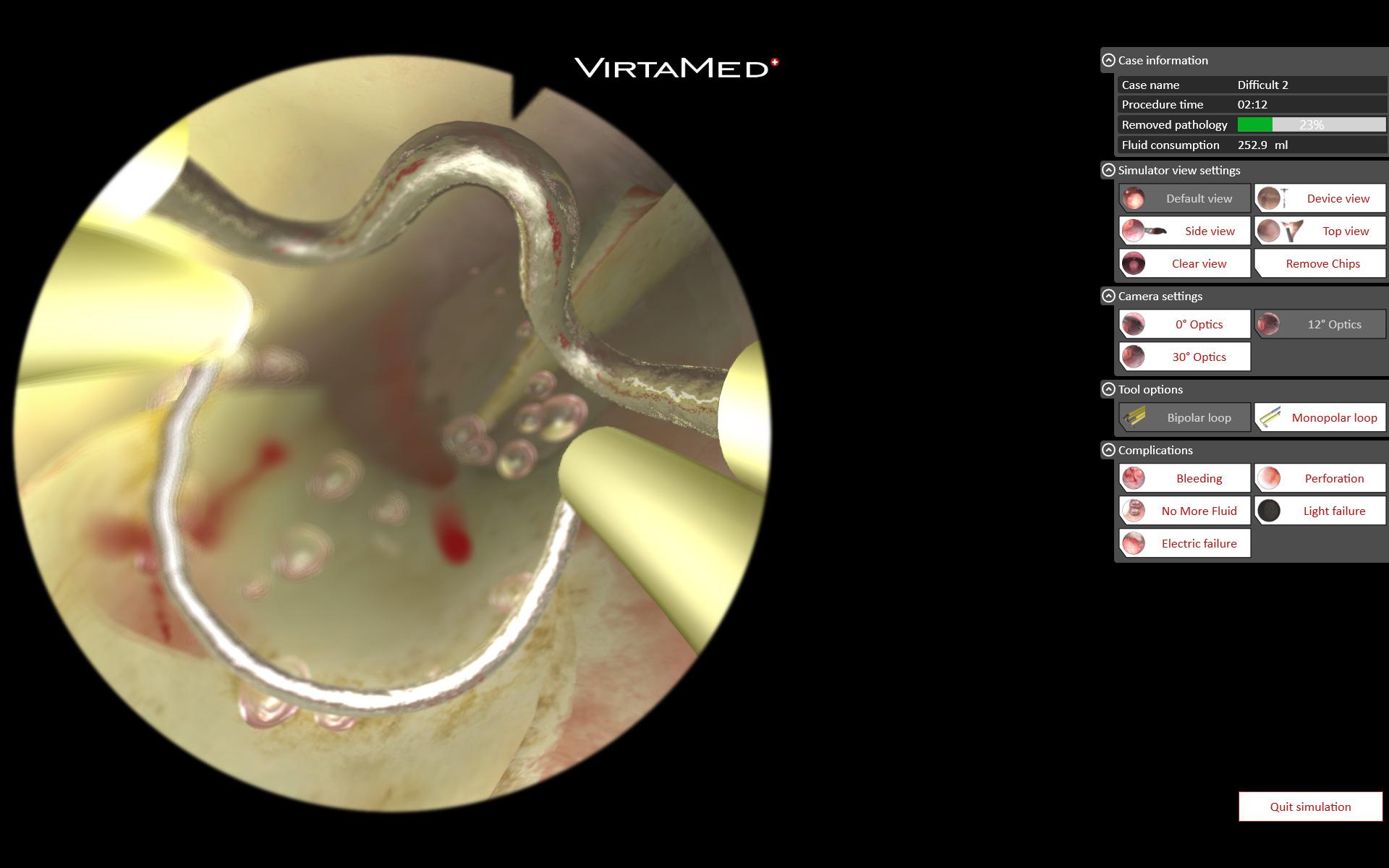
GynoS™ Hysteroscopy
A comprehensive, risk-free endoscopy training simulator that offers students a variety of pathologies and cases at all difficulty levels. Students use original medical instruments to practice treating virtual fibroids, establishing uterine distension, clearing viewing conditions, and safely handling loop electrodes and rollerballs for resection, coagulation, and endometrial ablation. For more experienced learners, there are patients with more serious gynecological pathologies, such as multiple polyps, intramural fibroids, uterine adhesions, or a septum. In the risk-free environment of simulation, students can also train on more advanced endoscopic techniques, such as reducing fluid inflow to reduce uterine distension and allowing intramural fibroids to expand into the cavity for easier resection.
LaparoS™ Gynecological laparoscopy
This module offers condensed diagnostic and surgical training cases for laparoscopy with highly realistic scenarios derived from both fertility surgery and other gynecological procedures. It can be combined with the GynoS™ platform for a full OB-GYN offering.
Platforms

Skill progression
Development and evaluation of a “simulator-based” ultrasound training program for university teaching in obstetrics and gynecology–the prospective GynSim study
This study addresses the challenges of ultrasound education in obstetrics and gynecology, focusing on the potential benefits of simulation techniques in medical training. Aiming to evaluate the impact of a structured simulator-based training program, this prospective, randomized, interventional study examines its effects on educational outcomes for 5th year medical students.
Preliminary Experience with Virtual Reality Simulation vs. Animal Model for Hysteroscopic Myomectomy Training
The HystSim™ Virtual Reality hysteroscopic trainer was felt to be at least equal to the ‘‘gold standard’’ pig bladder model for training in hysteroscopic myomectomy with the additional advantages of reproducibility and measurement of results. Further studies comparing modalities and relating results to operating room performance are warranted.
Establishing construct validity of a virtual-reality training simulator for hysteroscopy via a multimetric scoring system
The aims of this study are to determine construct validity for the HystSim™ virtual reality (VR) training simulator for hysteroscopy via a new multimetric scoring system (MMSS) and to explore learning curves for both novices and experienced surgeons.
VirtaMed services
Connect
VirtaMed Connect is your all-in-one online platform, securely storing course data in the cloud for 24/7 access. With Connect, course directors effortlessly track resident progress, evaluate cohort and individual performance, and deliver targeted feedback. Plus, it simplifies the implementation of new courses, saving you valuable time while monitoring student progress.
Proficiency development
Technology is transforming medical education and training. VirtaMed's Training and Education team is skilled at developing training programs and optimally integrating active learning solutions into the learning journey.
Service & support
With a Net Promotor Score of more than 90, VirtaMed Services and Support team provides ongoing support, with a proven track record to resolving customer issues swiftly and effectively, ensuring seamless and hassle-free technology experiences.
Supporters
Factsheets & validation
Get more details about the most realistic ob-gyn simulator.