
UroS™
Comprehensive urology training simulator with unmatched realism: real graphics, real instruments, real feel.
Our expertise
Modules
UroS™ BPH laser module
This BPH education module allows trainees to gain experience in removing prostatic tissue with ThuLEP and HoLEP. The prostate sizes range from 55-90 grams. Trainees learn how to use different power settings and laser techniques such as vaporization, enucleation, or vaporesection. Safe handling of the laser fiber without any harm for the virtual patient is one of the main learning goals of this laser BPH training.
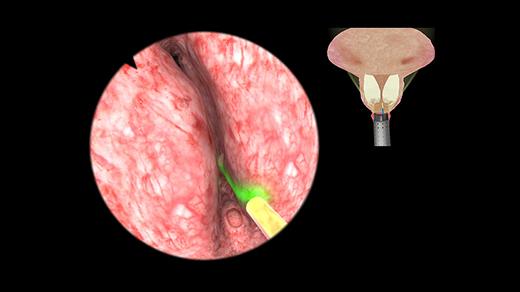
UroS™ TURB Module
4 patients with different multiple papillary and solid tumors offer the trainee the opportunity to perform a complete TURB procedure in a safe environment without involving patient related risk. The goal of this urologic surgery is to remove bladder tumors in various locations, ranging from easily accessible to locations that are more difficult to reach. Managing complications is also one of the learning objectives: bleedings have to be controlled, and the risk of perforating the thin bladder wall has to be avoided.
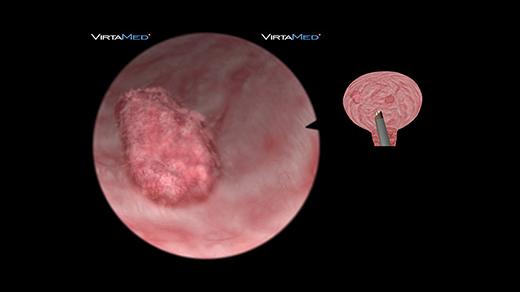
UroS™ TURP basic skills module
The basic skills module covers all aspects of a complete TURP procedure: the trainee learns how to safely enter the urethra, do a proper visualization of the bladder, and identify important landmarks such as verumontanum and ureteral orifices. Crucial learning objectives of this module also include efficient coagulation of bleedings to avoid severe complications later on.
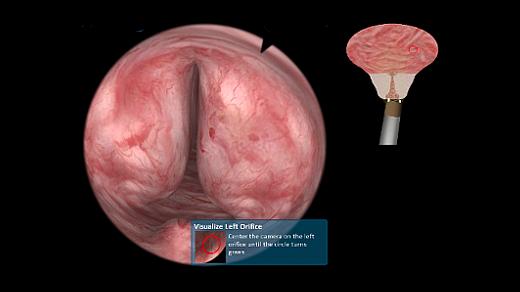
UroS™ TURP full procedure module
This module contains eight different patient cases for full TURP procedures to acquire all skills necessary to safely perform a complete transurethral resection of the prostate. The TURP courses teach an understanding of the anatomic landmarks, depth perception and hand-eye coordination during urologic surgery, and how to control flow and bleedings for a clear view during the BPH procedure.
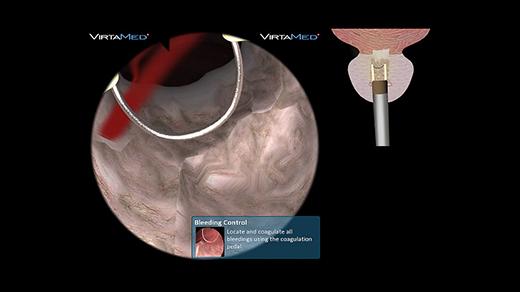
Platforms


Partnership
VirtaMed services
Connect
VirtaMed Connect is your all-in-one online platform, securely storing course data in the cloud for 24/7 access. With Connect, course directors effortlessly track resident progress, evaluate cohort and individual performance, and deliver targeted feedback. Plus, it simplifies the implementation of new courses, saving you valuable time while monitoring student progress.
Proficiency development
Technology is transforming medical education and training. VirtaMed's Training and Education team is skilled at developing training programs and optimally integrating active learning solutions into the learning journey.
Service & support
With a Net Promotor Score of more than 90, VirtaMed Services and Support team provides ongoing support, with a proven track record to resolving customer issues swiftly and effectively, ensuring seamless and hassle-free technology experiences.
Factsheets & validation
Learn more about the most advanced and comprehensive urology simulation platform available

