Medical training simulators
Your goal: shorter learning curves and seamless transfer of skills to the operating room. Virtual reality simulators are available 24/7 and accelerate the time needed to gain competency. Original instruments provide a complete training experience and optimally prepare users for the real procedure. Bring a real competitive edge to your training program!
Our expertise
Incorporating high-fidelity surgical simulators into medical training curricula for laparoscopy delivers many benefits for healthcare professionals. VirtaMed’s advanced simulators offer hyper-realistic simulation, with original instruments and authentic patient positioning. VirtaMed simulators improve surgeon proficiency faster in a risk-free, measurable, and motivating environment. VirtaMed's modular product range for various specialitites means lower-cost and scalable training environments. This technology facilitates a structured and standardized approach to training, ensuring that medical professionals are well-prepared for the challenges they may encounter in the operating room. Overall, using mixed-reality simulators represents a crucial advancement in medical education, enhancing the quality and safety of training while ultimately improving patient outcomes.
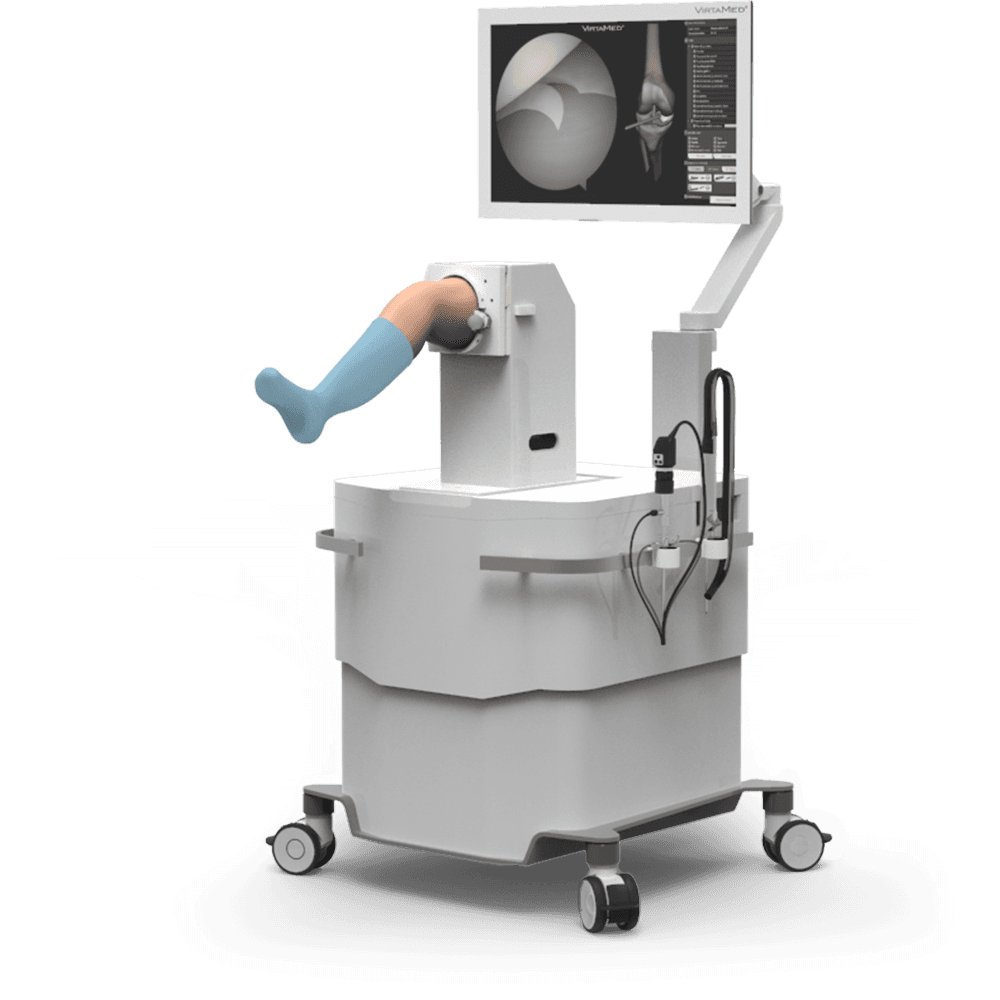
Orthopedics
Meet the VirtaMed ArthroS™ knee, shoulder, hip, and ankle simulator for arthroscopic skill training using an original arthroscope, camera and other surgical instruments adapted for simulation.
Robotic surgery
Our robotic surgery simulator enables independent, hands-on training with lifelike realism, helping surgeons build skills and transition confidently to the operating room.
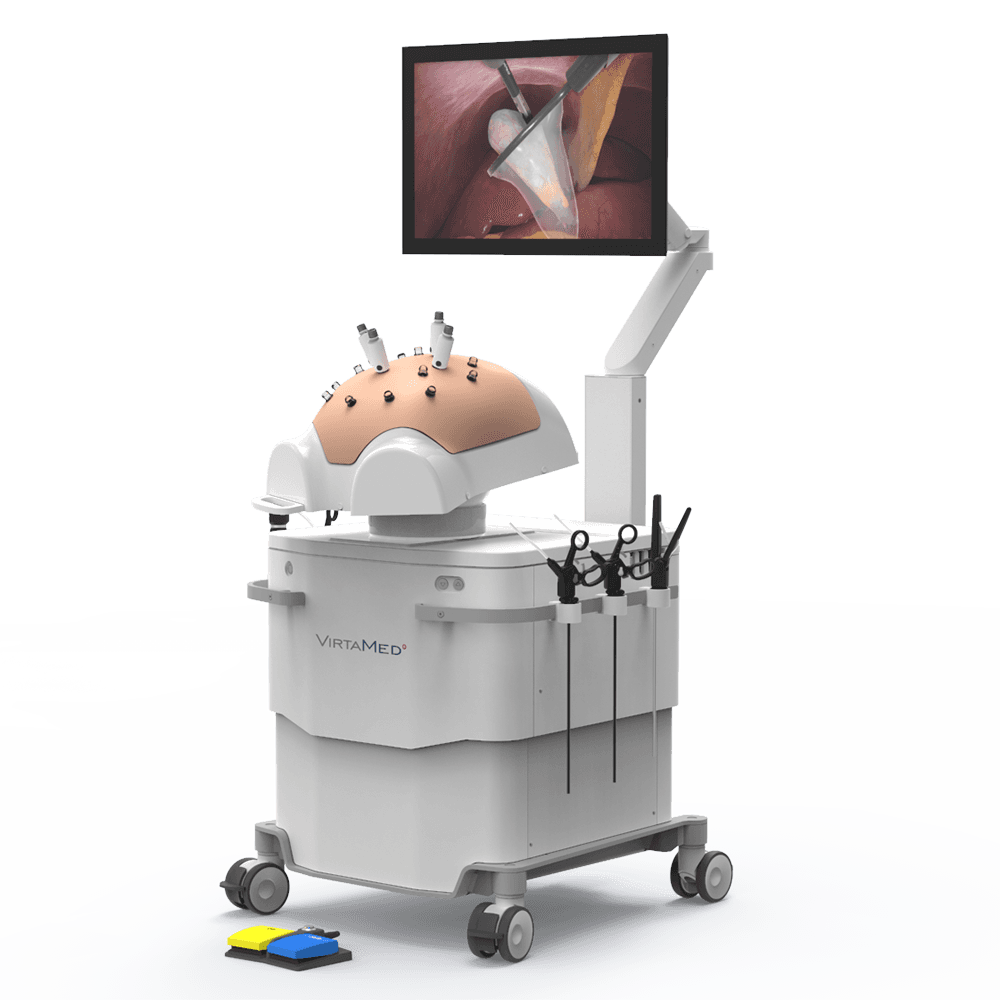
Laparoscopy
VirtaMed LaparoS™ brings an innovative approach to laparoscopic simulation, providing motivational training sequences in a highly realistic anatomical environment.
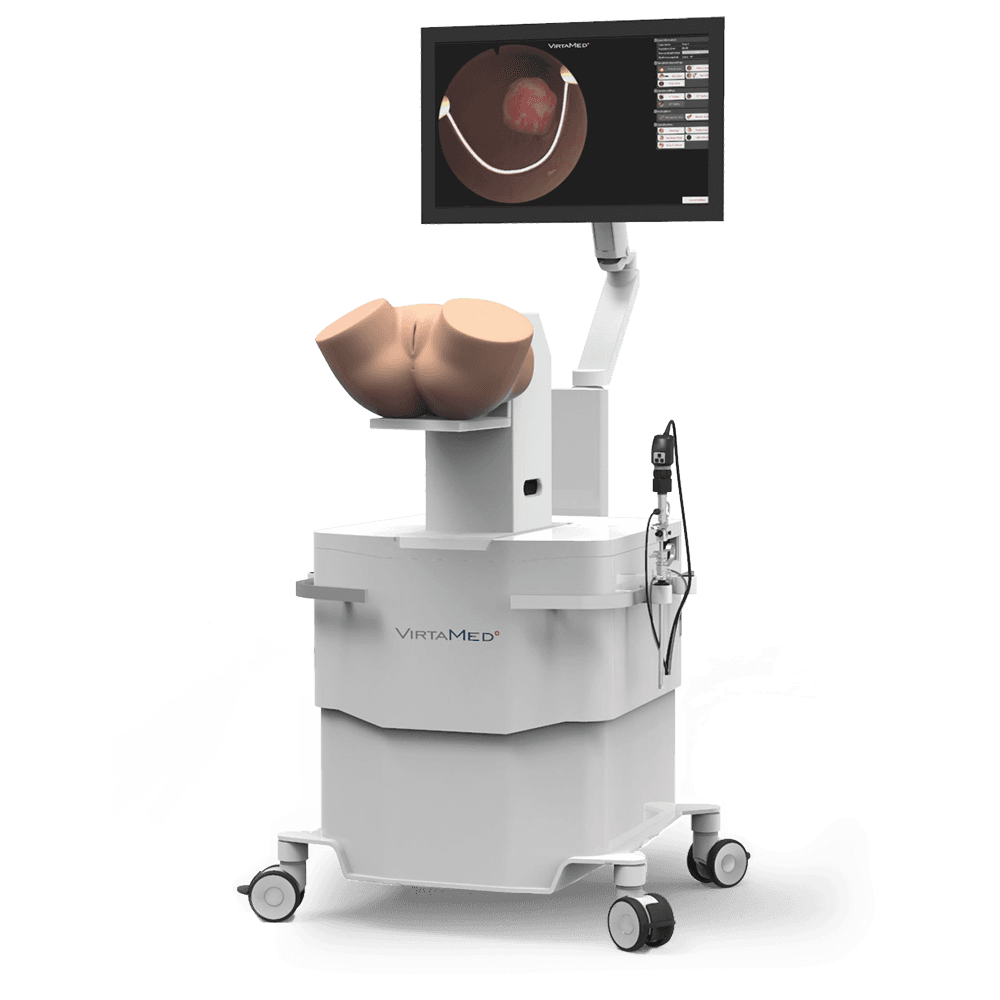
Obstetrics and Gynecology
VirtaMed GynoS™ provides life-like gynecology training at no risk to live patients. It is the most realistic virtual-reality simulator for obstetric ultrasound, IUD insertion, embryo transfer, and hysteroscopy.
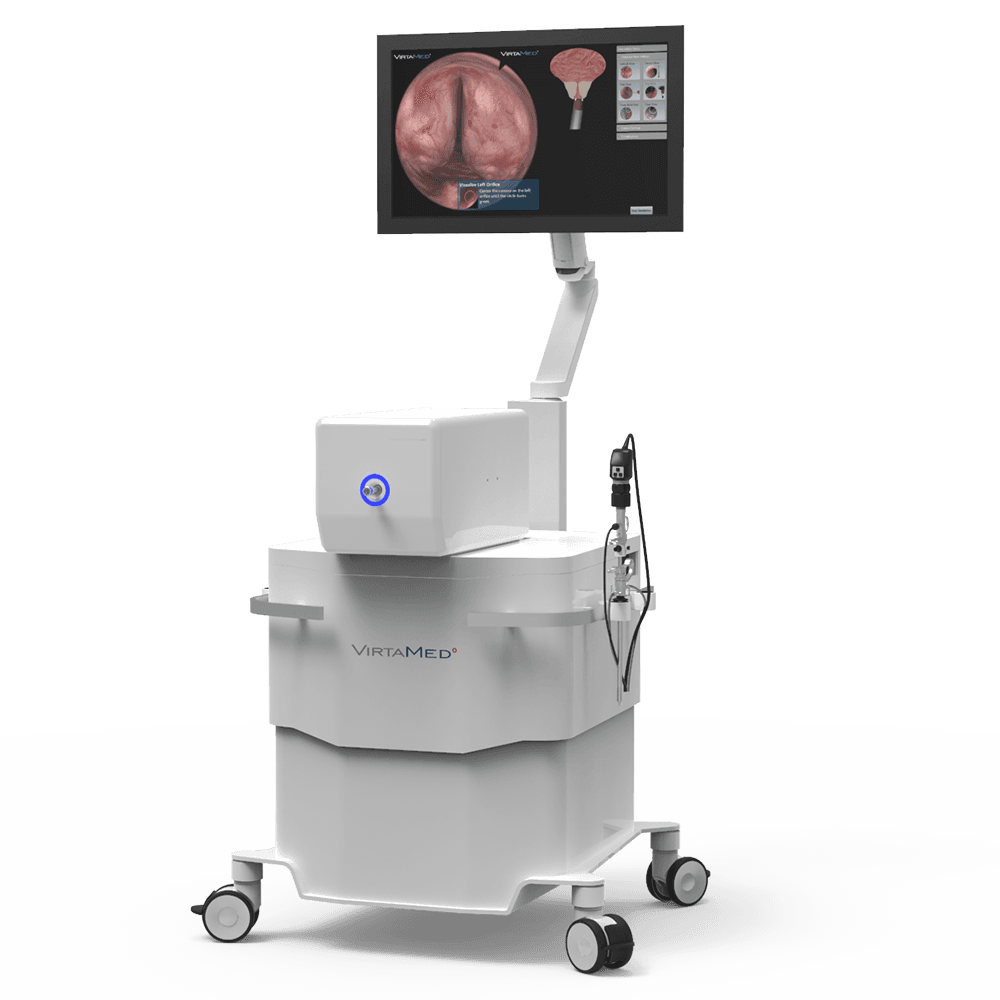
Urology
Learn more about the VirtaMed UroS™, which offers surgical training in urology, specifically operative TURP, TURB, morcellation, and laser BPH procedures.